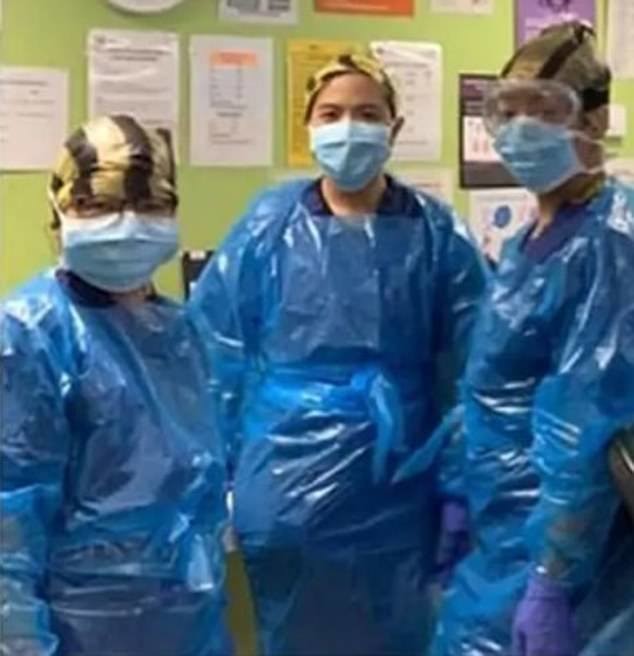
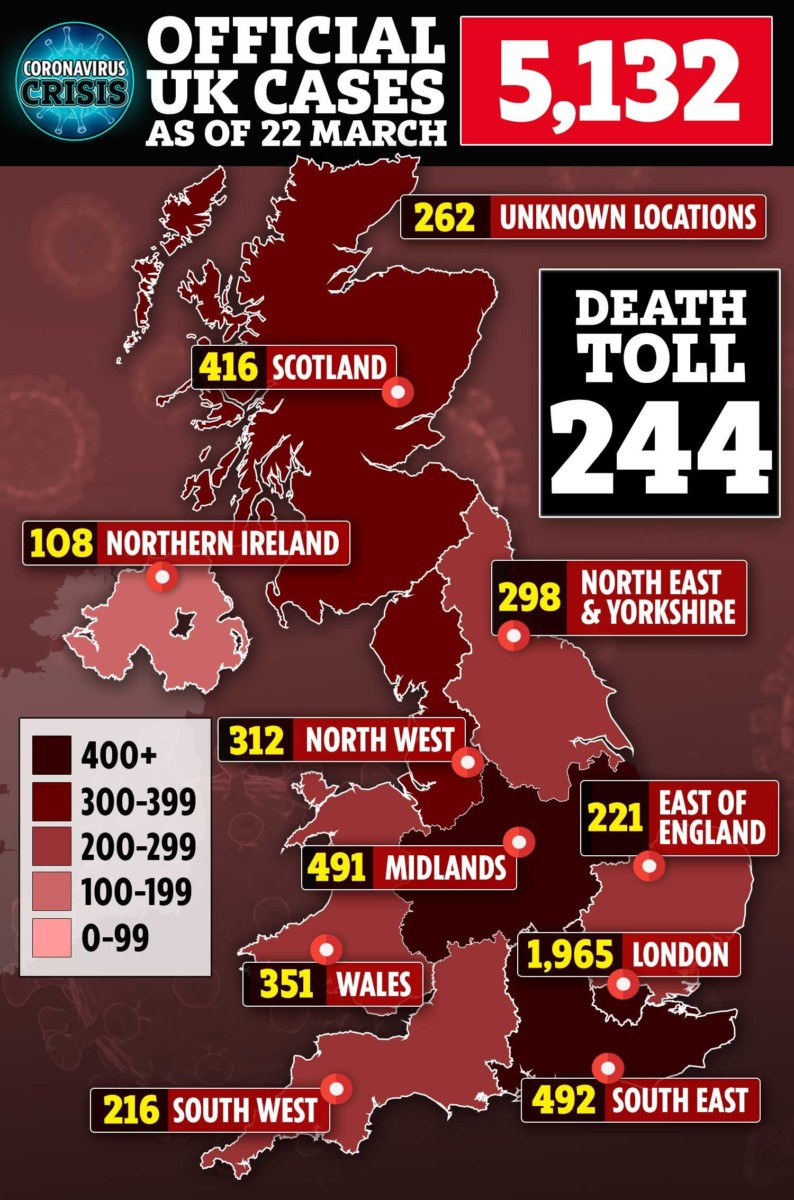
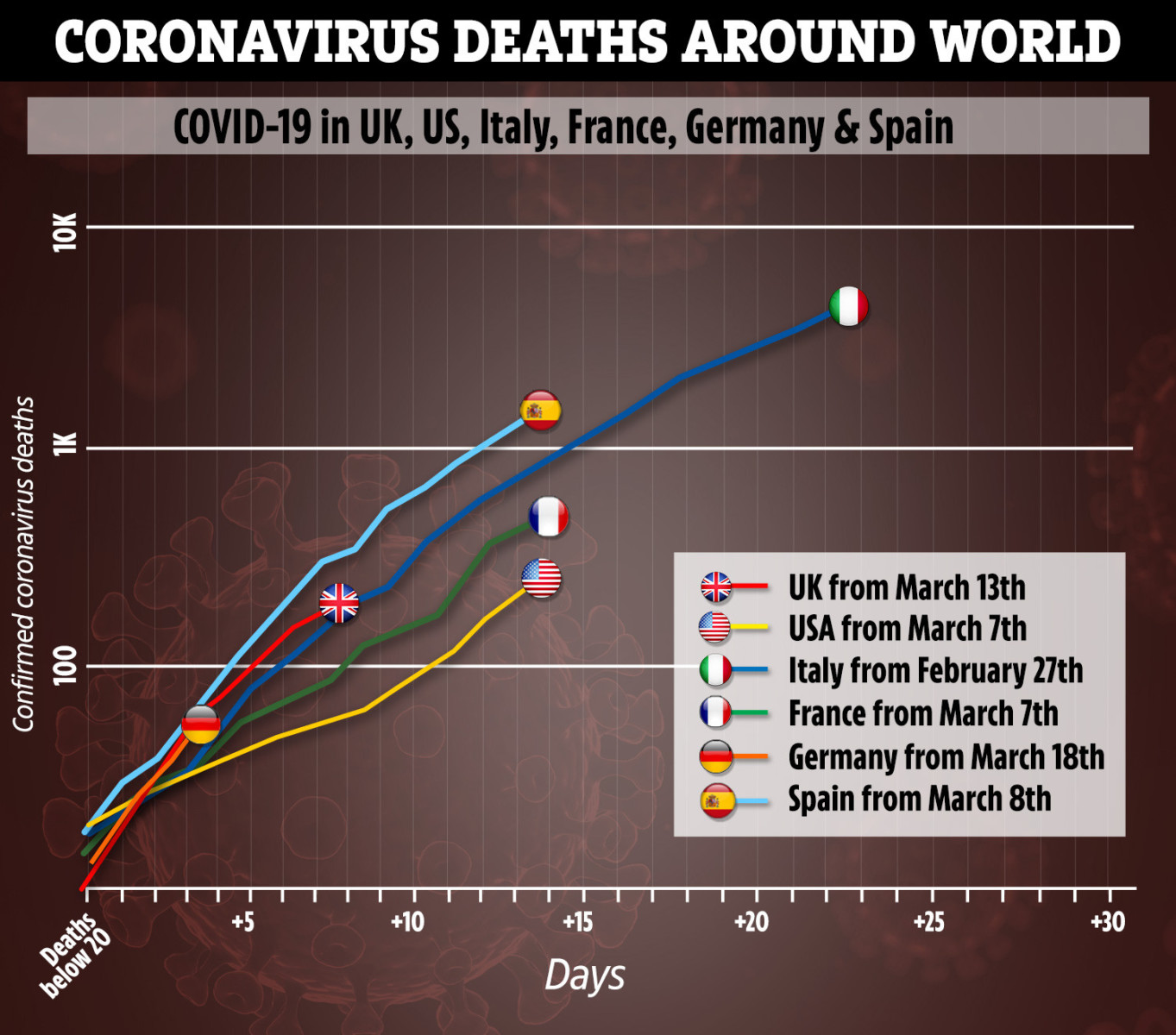
They fear they are putting their lives on the line because of shortages of equipment.

NHS staff are under constant pressure as the UK battles the coronavirus pandemic
And some are said to be fighting for their lives themselves after treating infected patients without adequate protective gear.
Chairman of the Doctors’ Association UK Dr Rinesh Parmar feared many medical staff would die.
He said: “We have had doctors tell us they feel like lambs to the slaughter, that they feel like cannon fodder. GPs tell us that they feel absolutely abandoned.
“We are all pleading with Boris Johnson that they really look into arranging the vital personal protection equipment that all of us need on the NHS front line.
“Frontline doctors have been telling us for weeks that they do not feel safe at work.
“Intensive care doctors and anaesthetists have told us they have been carrying out the highest-risk procedure, putting a patient on a ventilator, with masks that expired in 2015.
“Paediatricians have told us their stock of protective glasses and masks will run out in 48 hours, including in special-care baby units.”
He spoke out as it emerged a staff nurse is in intensive care battling the virus. Mum-of-three Areema Nasreen, 36, is critically ill in Walsall Manor Hospital, West Midlands, where she has worked for 16 years.
Her sister Kazeema said: “She is on a ventilator and fighting for her life. I want everyone to know how dangerous this is. My sister is only 36 and is normally fit and healthy.
“People are not taking this seriously enough. She is young — it is not just the elderly who are at risk.”
FIGHTING FOR THEIR LIVES
Yesterday, HOAR revealed three junior doctors in the same hospital had fallen ill with the virus.
The three, all aged 30, have been placed on ventilators and are being treated in London.
An ear, nose and throat consultant is also fighting for his life in hospital after being infected with coronavirus, which he is thought to have caught during a routine appointment with a patient. The 52-year-old, from the Midlands, had been fit and well but is on a life-support machine.
One central London hospital consultant, who does not work in intensive care, said many staff had no personal protective equipment.
He added: “There’s not even basic normal surgical masks, hand wash and hand gel in many areas where it’s really needed.”
The doctor said one NHS worker was reduced to “driving around B&Qs buying up dust masks”.
He added: “It’s like sending us to put out a huge fire wearing no protective equipment, while asking everyone else to stay at home.”
Dr Lisa Anderson, a consultant cardiologist at St George’s Hospital in South London, said staff risked “cross-infecting everybody” owing to the lack of kit — and much of the equipment that is being handed out not meeting world health guidelines.
HOSPITALS UNDER STRAIN
Hospitals are scrambling to cope with the spike in infected patients, many of them struggling to breathe.
Operating theatres are being frantically converted into intensive care wards while other patients are being discharged to make way for a surge in coronavirus cases.
But such is the concern over lack of ventilators that Christine Middlemiss, the UK’s chief veterinary officer, has written to every practice in the country asking for an inventory of their respiratory equipment.
Equine clinic boss Angela Walsh, from Henley-in-Arden, Warwicks, said: “This brings home how serious this pandemic is. Never before have the vets of Britain been asked to provide equipment for humans.”
‘TSUNAMI COMING SOON’
An intensive care specialist in South London said his hospital had saved a dozen patients in the past week.
But they warned: “A tsunami is coming soon and there will be a time when we won’t be able to help everyone who needs an intensive care bed.
Consultant anaesthetist Dr Tom Dolphin, a British Medical Association spokesman, said intensive care specialists would soon need to make difficult decisions on who to save.
He said hospitals that were full would transfer patients to others with intensive care space — but soon there could be no beds anywhere.
He added: “We’re going to find ourselves at the point where decisions are going to get harder and harder.
“It won’t be on age and it never has been, it will be on chance of survival.” But Jason Leitch, the national clinical director of healthcare quality and strategy, insisted: “The supply chain is robust and now the distribution will get better over the next few days.”
Meanwhile, a paramedic working all hours battling the pandemic has been evicted over virus fears.
Joseph Hoar was told by his landlady by text to pack up after she claimed it was “only a matter of time” before he brought home the bug.
The South Western Ambulance Service worker was inundated with offers of help after he posted online.
On a brighter note, Royal Glamorgan Hospital staff danced and sang to Olly Murs as A&E was deep-cleaned. Nurse Donna Walker said: “We are determined to remain positive.”